Living with constant back pain feels like your body is holding you back from the life you want to live. Simple things- like playing with your kids, running errands, or just getting through the day, become challenges you never expected.
Spondylolisthesis might be behind your constant struggles!
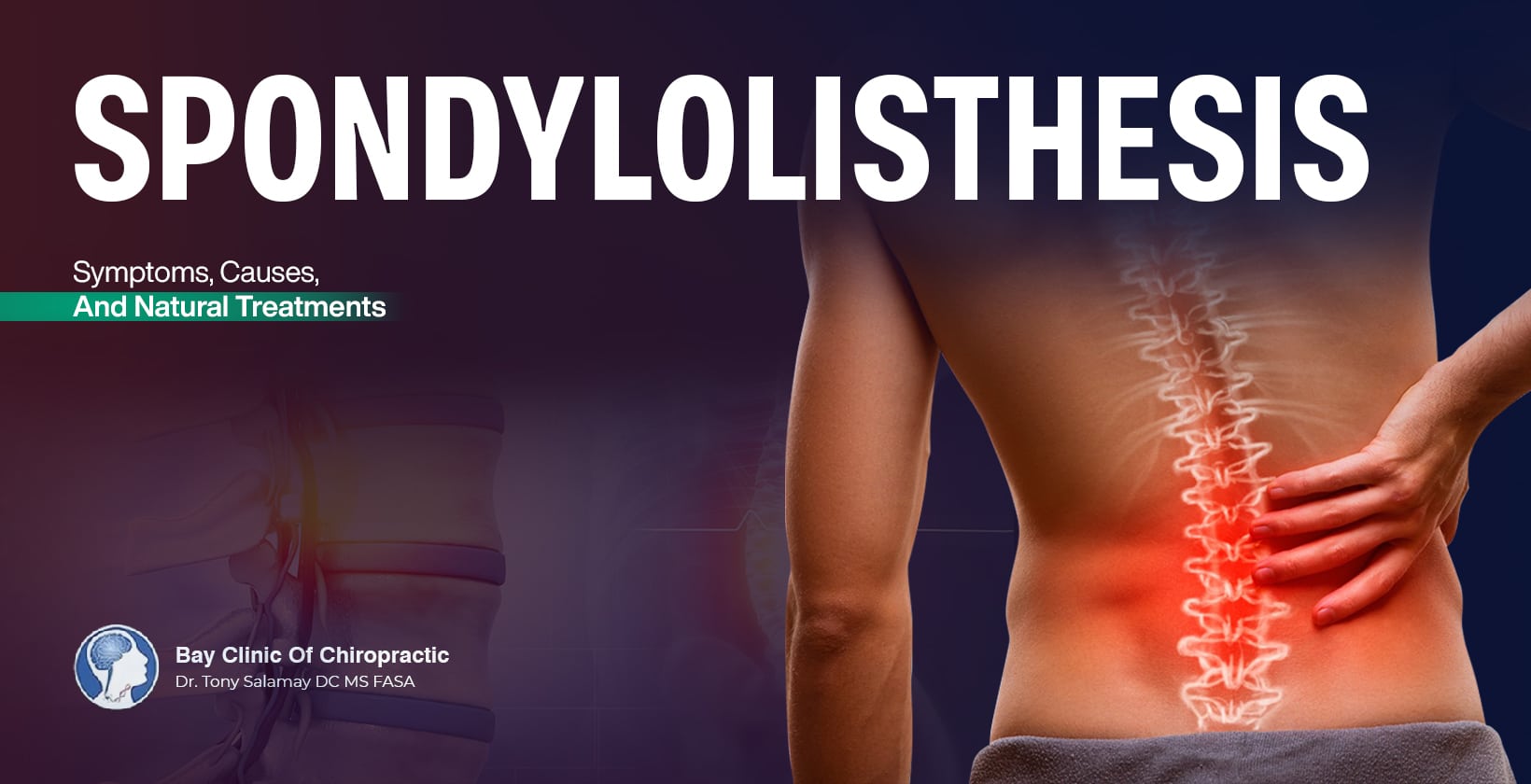
Spondylolisthesis happens when one of your spinal bones has slipped out of place, creating pain, stiffness, and even nerve issues.
You might notice symptoms like:
- Persistent lower back pain that worsens when you’re active.
- Tight, stiff muscles that limit your ability to move freely.
- Numbness or tingling in your legs makes it hard to feel comfortable.
We often associate back problems with older people. However, research by Dr. Steven Tenny from the University of Nebraska Medical Center, NE, USA, states “Isthmic spondylolisthesis is more common in the adolescent and young adult population but may go unrecognized until symptoms develop in adulthood.” This highlights the importance of getting a proper assessment and starting non-invasive treatment.
But there is hope, and you have options!
In this article, you’ll explore natural treatments for spondylolisthesis that can help, from chiropractic care and functional medicine to herbal remedies and lifestyle changes like yoga. These approaches work together to reduce pain, restore movement, and get you back to living fully.
Keep reading to learn more about spondylolisthesis and how to treat it naturally!
What Is Spondylolisthesis?
Spondylolisthesis is when a vertebrae (spinal bone) slips over the one below it. This can happen anywhere in your spine but is often seen in the lower back (lumbar spondylolisthesis). The most common symptoms are pain and stiffness and it often results from wear and tear, trauma, or congenital conditions.

The severity of slippage varies, with some cases causing minor discomfort while others lead to nerve irritation or restricted movement. Doctors grade the condition from grade 1 spondylolisthesis (mild) to grade 4 spondylolisthesis (severe) based on how far the vertebra has moved.
Spondylolisthesis affects people of all ages but is more common in older adults due to degenerative changes. Athletes in high-impact sports may also be at risk. Treatment ranges from rest and physical therapy to bracing and, in severe cases, surgery.
However, many cases improve with natural methods, including lifestyle adjustments and exercises. The type of spondylolisthesis you have can guide the best course of action.
Types of Spondylolisthesis
There are several types of spondylolisthesis which include:
- Isthmic: Tiny stress fractures weaken part of the vertebra, causing it to slip forward. This is often seen in athletes with repetitive motions.
- Degenerative: Spinal wear and tear, including arthritis, deteriorates discs and joints, making vertebrae unstable and prone to slipping.
- Congenital: Malformations in the spine present at birth increase the likelihood of vertebral instability and misalignment over time.
- Traumatic: Direct injuries, like falls or car accidents, damage the vertebrae or supporting structures, leading to slippage.
- Pathologic: Diseases like osteoporosis, cancer, or infections weaken vertebrae, making them unable to support normal alignment.
- Post-Surgical: Surgery complications, such as destabilization of spinal structures, can lead to vertebral slipping. For example, spinal fusion surgery may place additional stress on adjacent vertebrae, leading to instability over time.
Find natural relief from spondylolisthesis at Bay Clinic of Chiropractic. Book your consultation today to reduce pain and restore mobility.
What Are The Risk Factors Of Spondylolisthesis?

Certain factors can contribute to the risk of developing spondylolisthesis. Those risk factors are:
- Age: Older adults are more prone to degenerative spondylolisthesis due to wear and tear on spinal discs and joints.
- Athletic Activities: High-impact sports, like gymnastics, football, or weightlifting, increase the risk of stress fractures in the spine.
- Genetics: A family history of spondylolisthesis or naturally weak spinal structures may increase your likelihood of developing the condition. Certain inherited traits, such as naturally weaker spinal structures or connective tissue disorders, may increase susceptibility to vertebral slippage.
- Previous Spinal Injuries: Trauma from falls, accidents, or surgeries can weaken or destabilize the spine, leading to vertebral slippage.
- Gender: Women are at higher risk, especially postmenopause, due to hormonal changes and a higher likelihood of osteoporosis. A study by Dr. Thomas Andersen from the Aarhus University Hospital, Denmark shows that “Degenerative spondylolisthesis has been reported to be 4-5 times more common in women than in men,”
- Congenital Conditions: Birth defects that affect the spine, like abnormal vertebral formation, can predispose individuals to this condition.
- Obesity: Excess body weight puts additional stress on the spine, increasing the chances of instability and slippage.
- Occupation: Jobs that involve heavy lifting, repetitive bending, or prolonged standing, can strain the spine, leading to spondylolisthesis.
What Are The Symptoms Of Spondylolisthesis?

The symptoms of spondylolisthesis include:
- Lower Back Pain: Pain worsens with physical activity and improves with rest. It may feel sharp, dull, or radiating.
- Leg pain, numbness, or tingling: Compression of spinal nerves can cause discomfort or altered sensation in the things, buttocks, or calves, also known as sciatica.
- Tight Hamstrings: The muscles in the back of your thighs may feel stiff, reducing flexibility and making movement harder.
- Reduced Mobility: Prolonged standing, walking, or bending can aggravate symptoms, limiting your ability to stay active.
What Causes Spondylolisthesis?
Here are the causes of spondylolisthesis:
- Stress Fractures: Repeated strain weakens the vertebra over time, often from sports like gymnastics, weightlifting, or football.
- Degeneration: Aging or arthritis reduces the spine’s ability to absorb shock, leading to slippage as discs and joints weaken.
- Trauma: Accidents or injuries can directly damage vertebrae, ligaments, or discs, destabilizing the spine and causing slippage.
- Birth Defects: Some people are born with improperly formed vertebrae, which makes the spine less stable and more likely to slip.

Natural Treatments For Spondylolisthesis
Spondylolisthesis can often be managed through natural treatments that relieve pain, improve mobility, and strengthen your spine. These methods reduce stress on the affected vertebrae and enhance overall spinal health. While severe cases may require medical intervention, many individuals find significant relief by adopting holistic approaches.
These treatments target the pain and address the underlying causes, such as weak muscles or poor spinal alignment. With consistency and the right approach, you can manage spondylolisthesis effectively and maintain a better quality of life.
Chiropractic Care
Chiropractic care is a non-invasive, natural approach to managing spondylolisthesis. It focuses on improving spinal alignment, reducing pain, and enhancing overall function.
Chiropractors use a combination of therapies to relieve stress on the affected vertebrae, improve mobility, and strengthen supporting muscles.
These therapies aim to restore balance to your spine and help you maintain better posture and movement in daily life.
Spinal Adjustments
Chiropractors use gentle, precise spinal adjustments to realign misaligned vertebrae and reduce nerve pressure. These adjustments can help restore normal joint function, improve posture, and relieve pain associated with spondylolisthesis. Adjustments are customized based on your condition’s severity to ensure safety and effectiveness.
Over time, regular adjustments may help you manage spondylolisthesis symptoms and promote spinal stability.
Soft Tissue Therapy
Soft tissue therapy focuses on relaxing tight muscles, relieving tension, and improving blood flow around the affected area. Techniques like massage, myofascial release, or trigger point therapy reduce stiffness, ease discomfort, and enhance flexibility. This therapy helps alleviate the muscle imbalances and spasms often associated with spondylolisthesis.
Postural Guidance
Proper posture reduces spinal stress and supports recovery. Chiropractors teach techniques to maintain a neutral spine while sitting, standing, or lifting. They may suggest ergonomic changes to your workspace or sleeping habits to promote better alignment and prevent the worsening of the condition.
Strengthening and Flexibility Exercises
Targeted exercises strengthen your core and back muscles to support your spine and prevent further displacement of your spine bones. Flexibility exercises improve mobility and reduce stiffness, making daily activities easier. Chiropractors guide you through customized routines that you can safely perform at home or under supervision. These exercises form a key part of long-term management for spondylolisthesis.
Functional Medicine
Functional medicine provides a personalized, holistic approach to managing spondylolisthesis by addressing the root causes of pain and spinal instability. It focuses on evaluating your overall health, lifestyle, and habits to create a tailored plan to improve your condition and enhance spinal function naturally.
For people with spondylolisthesis, functional medicine examines lifestyle factors contributing to inflammation, spinal stress, and overall health. Practitioners assess your daily activities, work environment, posture, and movement patterns to identify areas that may exacerbate your condition. They provide specific strategies to reduce spinal strain, improve mobility, and support recovery.
Functional medicine also considers additional factors like environmental toxins and hormone imbalances. Reducing your body’s toxic load by supporting elimination in the liver and kidneys and addressing hormonal irregularities, such as cortisol (stress hormone) levels, can further enhance your body’s healing process.
A study by Dr. Zhongyu Li from the China Academy of Chinese Medical Sciences, Beijing, China, states that “natural products and dietary interventions have beneficial therapeutic effects on liver enzyme levels”, contributing to better liver function. Stress management techniques and improved sleep quality play essential roles in this approach, helping to reduce inflammation and promote spinal health.
Dietary Changes
Diet plays a key role in supporting spinal health and reducing inflammation. Eating the right foods can help your body repair and maintain tissues while avoiding certain foods can prevent inflammation that worsens pain and discomfort. A balanced diet focusing on nutrient-dense, whole foods may also enhance your overall energy and quality of life, helping you manage your condition better.

Here’s what to eat and what to avoid for spondylolisthesis:
Foods to Eat for Spondylolisthesis
- Fruits and Vegetables: Rich in antioxidants, vitamins, and minerals that reduce inflammation and promote tissue repair. Examples include leafy greens, berries, oranges, and broccoli.
- Whole Grains: Provide fiber and nutrients to reduce inflammation and support overall health. Opt for quinoa, oats, brown rice, and whole wheat.
- Lean Proteins: Support muscle repair and spinal stability. Include chicken, turkey, eggs, and plant-based options like lentils and beans.
- Healthy Fats: Reduce inflammation and support joint health. Sources include avocados, nuts, seeds, and olive oil.
- Hydrating Foods: Keep discs and tissues hydrated. Include cucumbers, watermelon, and soups alongside adequate water intake.
Foods to Avoid for Spondylolisthesis
- Processed Foods: High in trans fats and additives that increase inflammation. Examples include chips, fast food, and packaged snacks.
- Refined Sugars: They cause blood sugar spikes, increase inflammation, and worsen pain. Avoid candy, baked goods, and sugary drinks.
- Saturated Fats: These fats are found in fried foods and fatty meats, which contribute to inflammation and poor spinal health.
- Excess Salt: Too much salt can lead to dehydration and worsen inflammation. Reduce intake of salty snacks, processed meals, and added salt.
- Alcohol: Increases inflammation and can interfere with muscle recovery and overall spinal health.

Supplements
Supplements can complement a healthy lifestyle to manage spondylolisthesis symptoms. They support joint health, reduce inflammation, and promote bone strength, helping to alleviate pain and improve mobility. While supplements don’t directly cure spondylolisthesis, they may enhance your body’s ability to heal and maintain spinal health. Always consult a healthcare provider before adding supplements to your routine.
Here are our recommendations of supplements for spondylolisthesis:
Glucosamine and Chondroitin
Glucosamine and chondroitin are natural compounds in cartilage that cushions joints and supports mobility. Glucosamine helps maintain cartilage structure by stimulating its repair and reducing breakdown, while chondroitin improves cartilage elasticity and water retention. Together, they work synergistically to reduce joint inflammation and pain, which can benefit those with spondylolisthesis by improving joint function and mobility.
These compounds are commonly derived from shellfish or produced synthetically. Foods like bone broth also provide some natural sources. According to MedlinePlus, the recommended daily doses are 1500 mg of glucosamine and 800-1200 mg of chondroitin, which are taken in divided doses for better absorption. Regular use may help slow cartilage degeneration and relieve pain associated with spinal instability.
Omega-3 Fatty Acids
Omega-3 fatty acids are essential fats found in foods like fish, seeds, and nuts. They reduce inflammation by blocking inflammatory pathways in the body which helps alleviate pain and stiffness in conditions like spondylolisthesis. Omega-3s also improve blood flow to tissues, supporting recovery and spinal health.
Natural sources include fatty fish like salmon and mackerel, as well as flaxseeds, chia seeds, and walnuts. Fish oil supplements are a great option for concentrated doses of omega-3s. According to the National Institutes of Health, the recommended daily intake ranges from 1000-1600 mg of combined EPA and DHA (the active components of omega-3).
Regular supplementation helps improve overall joint and spinal health, but you should always consult a healthcare provider or a functional medicine practitioner to determine the correct doses for your specific needs.
Vitamin D and Calcium
Vitamin D and calcium are essential for maintaining strong, healthy bones. Calcium provides the building blocks for bone tissue, while vitamin D aids calcium absorption and bone remodeling. Together, they support spinal stability and help prevent further degeneration in individuals with spondylolisthesis.
Vitamin D is naturally synthesized in the skin through sunlight exposure, while dietary sources include fortified foods, egg yolks, and fatty fish. Calcium is found in dairy products, leafy greens, and fortified plant-based alternatives. According to the National Institutes of Health, the recommended daily intake for adults is 600-800 IU of vitamin D and 1000-1200 mg of calcium.
Supplementing both nutrients ensures optimal bone health and may help reduce spinal stress. Consistent intake supports overall spinal structure and can be an important part of managing spondylolisthesis.
Herbal Remedies
Herbal remedies offer a natural way to manage pain and inflammation caused by spondylolisthesis. Many herbs contain active compounds that help reduce discomfort, improve mobility, and support overall spinal health.
Options like devil’s claw, willow bark, and capsaicin are known for their anti-inflammatory and pain-relieving properties that relieve pain related to spondylolisthesis. Keep reading to learn more about these natural remedies.
Devil’s Claw
Devil’s Claw is a plant native to southern Africa and is known for its anti-inflammatory and pain-relieving properties. Its active compound, harpagoside, helps reduce inflammation in the joints and surrounding tissues which can alleviate pain and stiffness associated with spondylolisthesis.
Devil’s Claw is available in several forms, including capsules, tinctures, tablets, and teas. Topical creams containing devil’s claw extract are also good for localized pain relief. Recommended doses of devil’s claw range from 600-1200 mg daily. It’s best to consult with a healthcare provider as it may interact with some medications such as blood thinners, blood pressure medications, or certain sedatives.
Willow Bark
Willow bark comes from the bark of the willow tree and contains salicin, a compound that turns into salicylic acid, similar to aspirin. It has natural pain-relieving and anti-inflammatory effects, making it a great natural remedy for back pain caused by spondylolisthesis.
You can use willow bark in capsules, teas, or liquid extracts. The bark is steeped in hot water for tea, while capsules provide a more concentrated dose. Typical daily doses range from 120-240 mg of salicin, depending on your needs. You should avoid willow bark if you are allergic to aspiration or taking blood-thinning medications.
Capsaicin
Capsaicin is the active compound found in chili papers that gives them their spicy flavor. It works by depleting a neurotransmitter called substance P, which transmits pain signals to the brain. Applying capsaicin to the skin reduces pain perception, making it an effective option for maintaining localized pain in spondylolisthesis.
Capsaicin is most commonly used in topical creams, gels, or patches. These products are applied directly to the affected area for pain relief. The strength of capsaicin creams can vary, with concentrations ranging from 0.025% to 0.1%.
Apply a small amount of the cream to your skin on the painful area two to four times daily, but avoid open wounds or irritated skin. You may feel a warm or tingling sensation that will subside with regular use.
Yoga
Yoga is a gentle and effective way to manage spondylolisthesis by improving flexibility, strengthening core muscles, and promoting better posture. Specific yoga poses, such as cat-cow or child’s pose, help stretch tight muscles, relieve tension, and stabilize the spine.
Strengthening the core muscles provides better support for the lower back, reducing stress on the affected vertebrae (spine bone) and preventing further slippage.
Yoga also improves balance and alignment, alleviating pain caused by poor posture or uneven weight distribution. Additionally, deep breathing and mindfulness can help reduce stress and gain mental clarity, contributing to muscle tension.
Heat and Cold Therapy
Topical heat and cold therapy is a simple way to manage pain and inflammation in spondylolisthesis.
Heat therapy helps relax tight muscles, improve blood circulation, and alleviate stiffness in the back. This can make movement easier and reduce discomfort. Warm baths, heating pads, or hot compresses are common options.
Cold therapy reduces inflammation and numbs pain by constricting blood vessels and lowering inflammation. Ice packs or a cold compress to the affected area can help after physical activity or during flare-ups.
For the best results, alternate between heat and cold therapy. Apply a hot compress for 15-25 minutes to loosen tight muscles, then a cold compress for 10-15 minutes to reduce swelling.
Rest and Activity Modification
Rest and activity modification are important components of managing spondylolisthesis, as they prevent further irritation to the affected vertebrae and allow for proper healing.
Resting during flare-ups reduces inflammation and relieves pressure on the spine. However, you should avoid prolonged inactivity, as it can lead to stiffness and weakened muscles that support the spine.
Activity modification involves identifying and avoiding movements that strain the lower back, such as heavy lifting, excessive bending, or high-impact exercises.
Spondylolisthesis Exercises To Avoid
When managing spondylolisthesis, some exercises can worsen symptoms or increase spinal instability. Avoiding these activities helps protect your spine and prevent spinal instability.
- Hyperextension Movements: Exercises like backbends, superman poses, or excessive arching of the back place stress on the lower spine and may worsen slippage.
- High-Impact Activities: Running, jumping, or contact sports create a repetitive force on the spine, increasing the risk of irritation and instability.
- Heavy Lifting: Weightlifting exercises, such as deadlifts and squats, can strain the lower back, especially with improper technique.
- Twisting Movements: Exercises involving excessive spinal rotation, like certain yoga poses or golf swings, can exacerbate nerve compression and pain.
Focus on low-impact exercises like walking, cycling, or swimming, which maintain mobility and promote circulation without stressing the spine. Maintaining a balance between rest and appropriate activity ensures the spine is supported and healing. This practice improves comfort and functionality over time.
Frequently Asked Questions
Can A Chiropractor Help With Spondylolisthesis?
Yes, chiropractors can help manage spondylolisthesis. They focus on reducing pain, improving mobility, and stabilizing your spine through non-invasive treatments. Chiropractors use gentle spinal adjustments, soft tissue therapies, and tailored exercises to strengthen spine-supporting muscles. These therapies help reduce pressure on nerves and improve overall function without surgery or medications.
What Is The Difference Between Spondylolisthesis And Spondylosis?
The difference between spondylolisthesis and spondylosis is that spondylolisthesis is when a vertebra slips out of place, while spondylosis involves age-related spinal degeneration. Spondylolisthesis causes instability and nerve pressure, while spondylosis leads to stiffness, pain, and reduced mobility due to disc and joint wear.
Can Ankylosing Spondylitis Cause Spondylolisthesis?
Ankylosing spondylitis (AS), a chronic inflammatory condition affecting the spine, does not directly cause spondylolisthesis but it is a risk factor. Prolonged inflammation and structural changes in the spine from AS may increase the risk of instability, potentially contributing to conditions like spondylolisthesis in rare cases.
Can Spondylolisthesis Be Reversed?
Spondylolisthesis cannot be fully reversed, as it involves structural changes in the spine. However, symptoms can be effectively managed through treatments like chiropractic care, supplements, light exercise, and lifestyle adjustments. These approaches can reduce pain, stabilize the spine, and improve your quality of life.
Conclusion
Spondylolisthesis can be challenging, but with the right combination of holistic treatments, you can manage symptoms, reduce pain, and improve mobility. From natural remedies like chiropractic care, functional medicine, and herbal therapies to lifestyle changes such as yoga, hot and cold therapy, and activity modification- there are many effective, non-invasive options available.
These approaches can help you regain control and enjoy a better quality of life by addressing the root causes and supporting your overall health. If you seek holistic guidance and expertise when dealing with spondylolisthesis, the Bay Clinic of Chiropractic is here to help!
At the Bay Clinic of Chiropractic in Panama City, Florida, Dr. Tony Salamay offers a unique blend of expertise in chiropractic care, functional medicine, and holistic therapies to provide a personalized approach to managing spondylolisthesis.
With a deep understanding of your condition, Dr. Salamay focuses on treating the underlying issues and helping you achieve long-term relief without relying solely on medications or invasive procedures.
If you’re ready to take the next step toward living pain-free and reclaiming your mobility, contact the Bay Clinic of Chiropractic at (850) 785-9372 or info@thebaydoctor.com today.
References
- Tenny S, Gillis CC. Spondylolisthesis. [Updated 2023 May 22]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK430767/
- Studnicka K, Ampat G. Lumbosacral Spondylolisthesis. [Updated 2023 Jul 22]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK560679/
- Emary, P. C., Eberspaecher, S. A., & Taylor, J. A. (2017). High-grade spondylolytic spondylolisthesis. The Journal of the Canadian Chiropractic Association, 61(2), 162–166.
- Denard, P. J., Holton, K. F., Miller, J., Fink, H. A., Kado, D. M., Yoo, J. U., Marshall, L. M., & Osteoporotic Fractures in Men (MrOS) Study Group (2010). Lumbar spondylolisthesis among elderly men: prevalence, correlates, and progression. Spine, 35(10), 1072–1078. https://doi.org/10.1097/BRS.0b013e3181bd9e19
- Burton MR, Dowling TJ, Mesfin FB. Isthmic Spondylolisthesis. [Updated 2023 Aug 8]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK441846/
- Konan LM, Davis DD, Mesfin FB. Traumatic Lumbar Spondylolisthesis. [Updated 2023 Jul 31]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK448159/
- Akkawi, I., & Zmerly, H. (2022). Degenerative Spondylolisthesis: A Narrative Review. Acta bio-medica : Atenei Parmensis, 92(6), e2021313. https://doi.org/10.23750/abm.v92i6.10526
- Andersen, T., Christensen, F. B., Langdahl, B. L., Ernst, C., Fruensgaard, S., Østergaard, J., Andersen, J. L., Rasmussen, S., Niedermann, B., Høy, K., Helmig, P., Holm, R., Egund, N., & Bünger, C. (2013). Degenerative spondylolisthesis is associated with low spinal bone density: a comparative study between spinal stenosis and degenerative spondylolisthesis. BioMed research international, 2013, 123847. https://doi.org/10.1155/2013/123847
- Kalichman L, Kim DH, Li L, et al. Spondylolysis and spondylolisthesis: prevalence and association with low back pain in the adult community-based population. Spine. 2009 Jan;34(2):199-205. DOI: 10.1097/brs.0b013e31818edcfd. PMID: 19139672; PMCID: PMC3793342.
- da Rocha Lemos Costa, T. M., Borba, V. Z. C., Correa, R. G. P., & Moreira, C. A. (2022). Stress fractures. Archives of endocrinology and metabolism, 66(5), 765–773. https://doi.org/10.20945/2359-3997000000562
- Fakharian, E., Mohammadzadeh, M., Saberi, H. R., Fazel, M. R., Rejali, M., Akbari, H., Mirzadeh, A. S., & Mohammadzadeh, J. (2017). Spinal injury resulting from car accident: Focus to prevention. Asian journal of neurosurgery, 12(2), 180–184. https://doi.org/10.4103/1793-5482.152110
- Rubinstein, S. M., Terwee, C. B., Assendelft, W. J., de Boer, M. R., & van Tulder, M. W. (2012). Spinal manipulative therapy for acute low-back pain. The Cochrane database of systematic reviews, 2012(9), CD008880. https://doi.org/10.1002/14651858.CD008880.pub2
- Wu, Z., Wang, Y., Ye, X., Chen, Z., Zhou, R., Ye, Z., Huang, J., Zhu, Y., Chen, G., & Xu, X. (2021). Myofascial Release for Chronic Low Back Pain: A Systematic Review and Meta-Analysis. Frontiers in medicine, 8, 697986. https://doi.org/10.3389/fmed.2021.697986
- Huxel Bliven, K. C., & Anderson, B. E. (2013). Core stability training for injury prevention. Sports Health, 5(6), 514–522. https://doi.org/10.1177/1941738113481200
- Bland J. (2017). Defining Function in the Functional Medicine Model. Integrative medicine (Encinitas, Calif.), 16(1), 22–25.
- Li, Z., Wu, J., Zhao, Y., Song, J., & Wen, Y. (2024). Natural products and dietary interventions on liver enzymes: an umbrella review and evidence map. Frontiers in nutrition, 11, 1300860. https://doi.org/10.3389/fnut.2024.1300860
- Hannibal, K. E., & Bishop, M. D. (2014). Chronic stress, cortisol dysfunction, and pain: a psychoneuroendocrine rationale for stress management in pain rehabilitation. Physical therapy, 94(12), 1816–1825. https://doi.org/10.2522/ptj.20130597
- Birben, E., Sahiner, U. M., Sackesen, C., Erzurum, S., & Kalayci, O. (2012). Oxidative stress and antioxidant defense. The World Allergy Organization journal, 5(1), 9–19. https://doi.org/10.1097/WOX.0b013e3182439613
- Mielgo-Ayuso, J., & Fernández-Lázaro, D. (2021). Nutrition and Muscle Recovery. Nutrients, 13(2), 294. https://doi.org/10.3390/nu13020294
- Tristan Asensi, M., Napoletano, A., Sofi, F., & Dinu, M. (2023). Low-Grade Inflammation and Ultra-Processed Foods Consumption: A Review. Nutrients, 15(6), 1546. https://doi.org/10.3390/nu15061546
- Ma, X., Nan, F., Liang, H., Shu, P., Fan, X., Song, X., Hou, Y., & Zhang, D. (2022). Excessive intake of sugar: An accomplice of inflammation. Frontiers in immunology, 13, 988481. https://doi.org/10.3389/fimmu.2022.988481
- Agócs, R., Sugár, D., & Szabó, A. J. (2020). Is too much salt harmful? Yes. Pediatric nephrology (Berlin, Germany), 35(9), 1777–1785. https://doi.org/10.1007/s00467-019-04387-4
- Zhu, X., Sang, L., Wu, D., Rong, J., & Jiang, L. (2018). Effectiveness and safety of glucosamine and chondroitin for the treatment of osteoarthritis: a meta-analysis of randomized controlled trials. Journal of orthopaedic surgery and research, 13(1), 170. https://doi.org/10.1186/s13018-018-0871-5
- Chondroitin Sulfate: MedlinePlus Supplements. (2023). Medlineplus.gov. https://medlineplus.gov/druginfo/natural/744.html
- Glucosamine: MedlinePlus Supplements. (2024). Medlineplus.gov. https://medlineplus.gov/druginfo/natural/807.html#Dosage
- Krupa KN, Fritz K, Parmar M. Omega-3 Fatty Acids. [Updated 2024 Feb 28]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK564314/
- Khazai, N., Judd, S. E., & Tangpricha, V. (2008). Calcium and vitamin D: skeletal and extraskeletal health. Current rheumatology reports, 10(2), 110–117. https://doi.org/10.1007/s11926-008-0020-y
- Office of Dietary Supplements – Calcium. (2025). Nih.gov. https://ods.od.nih.gov/factsheets/Calcium-HealthProfessional/
- Office of Dietary Supplements – Vitamin D. (2025). Nih.gov. https://ods.od.nih.gov/factsheets/VitaminD-HealthProfessional/
- Gxaba, N., & Manganyi, M. C. (2022). The Fight against Infection and Pain: Devil’s Claw (Harpagophytum procumbens) a Rich Source of Anti-Inflammatory Activity: 2011-2022. Molecules (Basel, Switzerland), 27(11), 3637. https://doi.org/10.3390/molecules27113637
- Chrubasik, S., Eisenberg, E., Balan, E., Weinberger, T., Luzzati, R., & Conradt, C. (2000). Treatment of low back pain exacerbations with willow bark extract: a randomized double-blind study. The American journal of medicine, 109(1), 9–14. https://doi.org/10.1016/s0002-9343(00)00442-3
- Frerick, H., Keitel, W., Kuhn, U., Schmidt, S., Bredehorst, A., & Kuhlmann, M. (2003). Topical treatment of chronic low back pain with a capsicum plaster. Pain, 106(1-2), 59–64. https://doi.org/10.1016/s0304-3959(03)00278-1
- Wieland, L. S., Skoetz, N., Pilkington, K., Harbin, S., Vempati, R., & Berman, B. M. (2022). Yoga for chronic non-specific low back pain. The Cochrane database of systematic reviews, 11(11), CD010671. https://doi.org/10.1002/14651858.CD010671.pub3
- French, S. D., Cameron, M., Walker, B. F., Reggars, J. W., & Esterman, A. J. (2006). Superficial heat or cold for low back pain. The Cochrane database of systematic reviews, 2006(1), CD004750. https://doi.org/10.1002/14651858.CD004750.pub2