You’re exhausted during the day, but the night gives you no rest. You wake up gasping, snore loudly, or toss and turn without knowing why. Morning headaches, brain fog, and irritability follow you like a shadow.
Sleep apnea is a sleep disorder that causes your breathing to repeatedly stop and start while you sleep. These pauses happen when your airway becomes blocked or when your brain doesn’t send the right signals to keep you breathing. Either way, your body wakes up over and over, never getting the deep rest it needs.
Sleep apnea symptoms can include:
- Loud snoring that disrupts your sleep or someone else’s
- Waking up choking, gasping, or short of breath
- Dry mouth or sore throat in the morning
- Constant fatigue even after a full night in bed
- Trouble focusing, mood swings, or low energy
According to Dr. Evan Cumpston from Indiana University, IN, USA, the prevalence of sleep apnea ranges from 21-59% in the general population and patients with cardiac disease, respectively.
In this article, you’ll learn the types, causes, and symptoms of sleep apnea and how it affects your overall health. We’ll also dive into holistic solutions like chiropractic care, targeted supplements, and simple lifestyle changes that can make a real difference.
If you’re tired of waking up like you’ve stayed up all night, keep reading- there’s a better way to sleep.
What Is Sleep Apnea?
Sleep apnea is a disorder that causes your breathing to repeatedly stop and start during sleep. These pauses can last from a few seconds to over a minute and may occur many times throughout the night.
Each pause lowers your oxygen levels (hypoxia), putting pressure on your heart and brain. Even if you don’t fully wake up, these interruptions prevent deep, restful sleep. Many people with sleep apnea don’t know they have it, since the symptoms happen while they’re asleep.
Loud snoring, gasping for air at night, and waking up feeling tired despite sleeping for hours are common signs. Daytime fatigue, irritability, and trouble focusing also point to poor sleep quality caused by sleep apnea.
This condition can affect anyone, but it’s more common in men over 40, people who are overweight, those with a family history of sleep apnea, and individuals with narrow airways or chronic nasal congestion.
Without treatment, sleep apnea can raise your risk for serious health issues like high blood pressure and heart disease.
What Are The Types Of Sleep Apnea?
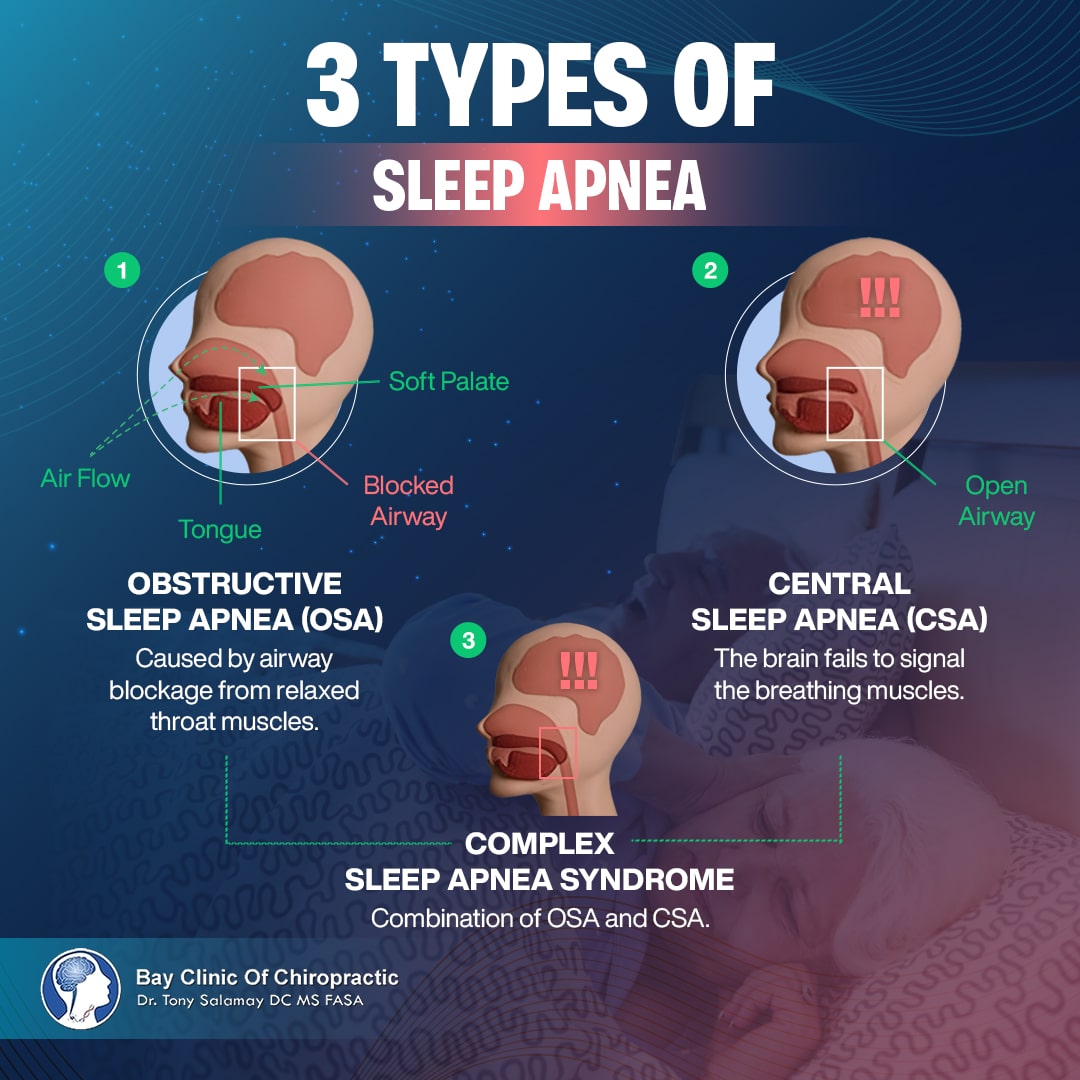
Sleep apnea comes in three main types, including:
- Obstructive Sleep Apnea (OSA): The most common type of sleep apnea. It happens when throat muscles relax too much during sleep, causing airway blockage. Snoring is a key symptom. A study by Dr. Jennifer M. Slowik from the Walter Reed National Military Medical Center, USA, shows that OSA is more prevalent in the Hispanic, African-American, and Asian populations.
- Central Sleep Apnea (CSA): Caused by the brain failing to signal the muscles that control breathing. This type usually doesn’t involve snoring but leads to poor sleep and fatigue. According to Dr. Abdul M. Rana from the CMH Lahore Medical College, University of Health Sciences, Lahore, Pakistan, “Central sleep apnea can result from heart failure, stroke, high altitude.”
- Complex Sleep Apnea Syndrome: A mix of both OSA and CSA. It often appears when someone starts CPAP therapy for OSA and develops central apnea symptoms.
What Are The Symptoms Of Sleep Apnea?

Sleep apnea symptoms often go unnoticed at first, especially if you sleep alone. Many signs show up at night, but the effects can carry into your day. Here are the symptoms of sleep apnea:
- Loud snoring: This is one of the most common and obvious signs. It usually gets worse over time and may be loud enough to disturb others.
- Gasping or choking during sleep: You might suddenly wake up feeling like you can’t breathe. These episodes can happen multiple times a night and often go unremembered.
- Pauses in breathing: Someone else may notice that you stop breathing for short periods while you sleep. These pauses can last several seconds and may happen repeatedly.
- Waking up with a dry mouth or sore throat: Breathing through your mouth all night can dry out your throat, leaving it sore or scratchy in the morning.
- Morning headaches: These happen because reduced oxygen levels during the night cause blood vessels in your brain to widen, triggering pain.
- Daytime fatigue: You may sleep for eight hours, but still feel completely drained. Interrupted sleep keeps your body from reaching the deep, restorative stages.
- Difficulty concentrating: Brain fog, slow thinking, and memory issues are common when your brain isn’t getting enough oxygen at night.
- Irritability or mood swings:Poor sleep quality can wear down your patience and increase feelings of anxiety or depression.
- Frequent nighttime urination: Getting up several times to use the bathroom may be linked to disrupted sleep cycles and stress on your heart and kidneys. According to Dr. Megan Doyle-McClam from the University of Tennessee College of Medicine Chattanooga, USA, “About 50% of patients with OSA have nocturia, and treatment of OSA improves it.”
Seeing these symptoms or risk factors in yourself? Don’t wait for your sleep or health to get worse. Take the next step and explore solutions that can help you breathe better, sleep deeper, and feel like yourself again. At Bay Clinic of Chiropractic, our holistic doctor in Panama City, FL can help you uncover the root cause and guide you toward lasting relief.
What Causes Sleep Apnea?

Here are the factors that may contribute to sleep apnea:
- Excess weight: Fat deposits around the neck and upper airway can block breathing during sleep. Obesity is one of the strongest risk factors for obstructive sleep apnea.
- Neck circumference: A thicker neck can narrow your airway. People with larger necks are more likely to develop breathing problems during sleep.
- A narrow airway: Some people naturally have a smaller throat or enlarged tonsils and adenoids. These can block airflow, especially in children.
- Aging: Muscle tone in the throat decreases with age. This makes the airway more likely to collapse during sleep.
- Family history: Genetics can affect your airway shape, sleep patterns, and risk for obesity, all of which raise the chance of sleep apnea.
- Smoking: Smoking inflames the airway and increases fluid retention. This makes it more likely for your airway to collapse while sleeping.
- Nasal congestion: Chronic stuffiness from allergies or a deviated septum makes it harder to breathe through your nose. This leads to mouth breathing and a higher risk of apnea.
- Use of alcohol or sedatives: These substances relax the muscles in your throat. That increases the chances of airway blockage during sleep.
- Medical conditions: Issues like hypothyroidism, heart failure, or polycystic ovary syndrome (PCOS) can raise your risk. They affect hormones, fluid balance, and airway control.
Holistic Remedies For Sleep Apnea
Holistic remedies aim to reduce sleep apnea symptoms by addressing root causes like inflammation, poor airway function, and overall health. These approaches often support or enhance conventional treatments rather than replace them.
Changes in diet, targeted supplements, body alignment, and stress management can improve sleep quality and breathing patterns. While not a cure, holistic care can help lower symptom severity and improve energy during the day.
The next sections break down the most effective natural strategies for managing sleep apnea.
Functional Medicine
Functional medicine takes a personalized approach to sleep apnea by looking at the underlying causes, not just the symptoms. It focuses on how different systems in your body interact and how imbalances can affect your breathing during sleep.
A functional medicine provider might test for hormone levels, inflammation markers, or nutrient deficiencies. Conditions like insulin resistance, low thyroid function, or chronic inflammation often contribute to sleep apnea and are commonly missed in standard care.
Treatment often includes a customized plan with dietary changes, lifestyle adjustments, supplements, and support for metabolic health. This approach can be especially helpful if you’ve tried conventional medicine without success.
Functional medicine doesn’t replace CPAP or surgery but adds a layer of holistic care aimed at long-term health improvements.
Dietary Changes
What you eat can influence how easily you breathe during sleep. Some foods trigger inflammation or cause fluid buildup, which narrows your airway and makes symptoms worse.

On the flip side, a nutrient-rich, anti-inflammatory diet can support open airways, improve metabolic function, and help you maintain a healthy weight. Your food choices also affect blood sugar, hormones, and digestion- all connected to how well you sleep.
The next sections break down which foods can help and which ones are best to avoid if you have sleep apnea.
Foods to Eat for Sleep Apnea
- Leafy greens: Rich in magnesium and antioxidants, these support muscle tone and reduce inflammation in the airway. Good choices include spinach, kale, and collard greens. Add a handful to your dinner or morning smoothie.
- Fatty fish: High in omega-3s and vitamin D, fish like salmon, mackerel, and sardines help lower inflammation and regulate sleep hormones. Aim for two servings per week, grilled or baked.
- Berries: Loaded with antioxidants, berries help reduce oxidative stress linked to sleep apnea. Blueberries, raspberries, and strawberries are easy to add to yogurt or oatmeal.
- Nuts and seeds: Provide healthy fats, magnesium, and fiber to support muscle function and keep blood sugar stable overnight. Try almonds, walnuts, chia seeds, or flax seeds as a snack or topping.
- Whole grains: Support steady blood sugar and reduce nighttime wakeups. Choose oats, quinoa, and brown rice. Swap out refined grains like white bread or pasta for these options.
- Lean protein: Helps maintain healthy muscle mass, including airway muscles, and keeps you full overnight. Go for skinless poultry, tofu, lentils, or eggs. Include a portion with dinner to avoid late-night snacking.
Foods to Avoid Sleep Apnea
- Processed meats: Bacon, sausage, and deli meats contain saturated fat and preservatives that increase inflammation and fluid retention. Swap them for lean proteins like grilled chicken or turkey.
- Refined carbs and sugars: White bread, pastries, candy, and soda spike blood sugar and contribute to weight gain. Replace them with whole grains and naturally sweet options like fruit.
- Fried foods: Greasy meals can slow digestion and worsen acid reflux, which is linked to sleep apnea. Choose baked or grilled versions instead, especially for dinner.
- Alcohol: Relaxes throat muscles and disrupts sleep cycles. Avoid drinking close to bedtime, or limit it to early evening in small amounts.
- Caffeinated drinks late in the day: Coffee, energy drinks, and cola interfere with falling and staying asleep. Stick to caffeine-free options after mid-afternoon.
Chiropractic Care
Chiropractic care can support better breathing during sleep by improving posture, spinal alignment, and nervous system function. Misalignments in the spine, especially in the neck and upper back, can affect how your airway opens during sleep.
When the spine is out of alignment, it can create tension or pressure that limits airflow or disrupts nerve signals involved in breathing. Gentle adjustments may help reduce that interference and promote more relaxed, open airways.
A case study by Dr. David E. Hopper from the National University of Health Sciences, Lombard, Illinois, USA, found that chiropractic adjustments, myofascial therapy, nutritional therapy, and ergonomic interventions helped improve symptoms of sleep apnea, as well as improved general health.
For people with obstructive sleep apnea, chiropractic care may also help reduce tension in the jaw, neck, and upper chest. Combined with other therapies, it can improve sleep quality and reduce the frequency of breathing disruptions.
Expert Chiropractor trained in upper cervical care or working with airway-focused techniques may offer added benefits when treating sleep apnea as part of a holistic plan.
Supplements
Targeted supplements may help manage sleep apnea by supporting muscle tone, calming the nervous system, and improving sleep quality. While supplements won’t cure sleep apnea, they can work alongside other treatments to ease symptoms.
Some nutrients are often low in people with sleep disorders, especially those tied to inflammation, stress, and poor recovery during sleep. When used correctly and under guidance from a healthcare provider, supplements may help reduce nighttime awakenings and improve how rested you feel in the morning.
The next sections cover specific supplements commonly used to support people with sleep apnea.
Vitamin D
Vitamin D is a fat-soluble vitamin that supports immune health, bone strength, and muscle function. It also plays a role in reducing inflammation and supporting the muscles that help keep your airway open during sleep. Low vitamin D levels are linked to a higher risk of sleep apnea and poor sleep quality overall.
Your body makes vitamin D when your skin is exposed to sunlight. You can also get it from foods like salmon, sardines, egg yolks, and fortified dairy or cereal products. According to the National Institutes of Health, the recommended daily amount of vitamin D is 600 IU for most adults and 800 IU for adults over 70 years old.
If you don’t get enough sun or have low levels, a supplement may help improve sleep quality and support overall airway health. Talk with your healthcare provider before taking a supplement to ensure proper dose.
Magnesium
Magnesium is an essential mineral involved in over 300 biochemical reactions in the body, including muscle and nerve function, blood sugar control, and blood pressure regulation. It plays a significant role in sleep by helping to regulate neurotransmitters that calm the nervous system, potentially improving sleep quality and reducing symptoms of sleep apnea.
Natural sources of magnesium include leafy green vegetables (like spinach and kale), nuts (such as almonds and cashews), seeds (like pumpkin and chia), whole grains, legumes, and dairy products. According to the National Institutes of Health, the recommended daily allowance for magnesium is 400-420 mg for adult men and 310-320 mg for adult women.
For sleep support, magnesium glycinate is often recommended due to its calming properties and better absorption. It’s advisable to consult with a healthcare provider before starting any supplementation, especially if you have underlying health conditions or are taking other medications.
Melatonin
Melatonin is a hormone naturally produced by your brain that helps regulate your sleep-wake cycle. It signals your body when it’s time to sleep and helps maintain a steady rhythm for rest. In people with sleep apnea, melatonin levels may be disrupted, leading to difficulty falling or staying asleep.
Supplementing with melatonin may help improve sleep onset and support better sleep quality. It can help reduce the fatigue and fragmented sleep associated with the condition.
Natural sources of melatonin include tart cherries, grapes, tomatoes, and walnuts, but these usually provide small amounts. Most people rely on supplements for noticeable effects.
According to Dr. Rosemary A. Savage from the Sampson Regional Medical Center, North Carolina, USA, melatonin supplements are typically used in doses of 0.1 to 10 mg taken before bedtime. Start with the lowest dose and talk to your healthcare provider if you’re using it regularly.
Herbal Remedies
Many people use herbs to improve sleep, calm the nervous system, and manage stress. In sleep apnea, certain herbal remedies may help you relax more deeply and get better sleep.
These herbs won’t fix airway blockages, but they can reduce symptoms like anxiety, restlessness, and light sleep. When combined with other treatments, they may help you feel more rested and improve your sleep quality.
You can take herbs as teas, capsules, or liquid extracts. Always check with your provider before starting any new herb, especially if you take medication or have other health issues.
The next sections highlight herbs often used to support sleep in people dealing with sleep apnea.
Valerian Root
Valerian root is an herbal remedy commonly used to support sleep and relaxation. It comes from the root of the Valeriana officinalis plant and has a long history of use in traditional medicine for treating insomnia, anxiety, and nervous tension.
Valerian may help people with sleep apnea by promoting deeper, more restful sleep and reducing the number of nighttime awakenings. It works by increasing levels of GABA (gamma-aminobutyric acid), a calming neurotransmitter that helps slow down brain activity and ease the nervous system.
You can find valerian in several forms, including capsules, tablets, tinctures, and herbal teas. Many people take it 30 minutes to two hours before bedtime.
While valerian is generally safe for short-term use, it may cause drowsiness or interact with sedatives. It’s best to start with a low dose and talk to a healthcare provider before using it regularly.
Chamomile
Chamomile is a gentle herb known for its calming effects and is one of the most popular natural remedies for sleep. It comes from the dried flowers of the Matricaria chamomilla plant and has been used for centuries to ease anxiety, support digestion, and promote restful sleep.
For people with sleep apnea, chamomile may help by reducing mild anxiety and promoting relaxation before bed. It doesn’t help airway obstruction, but it can make it easier to fall asleep and stay asleep through the night. Some studies suggest chamomile may also reduce inflammation, which can support overall respiratory health.
You can use chamomile in several forms, including tea, capsules, liquid extracts, and essential oils. Drinking a warm cup of chamomile tea about 30 to 60 minutes before bed is one of the most common ways to use it.
Chamomile is generally safe, but avoid it if you’re allergic to ragweed or similar plants.
Ashwagandha
Ashwagandha is an adaptogenic herb traditionally used in Ayurvedic medicine to help the body manage stress and promote balance. It comes from the root of the Withania somnifera plant and is well-known for its calming and restorative properties.
For people with sleep apnea, ashwagandha may help by lowering stress hormones like cortisol, improving your body’s ability to relax at night. It may also enhance sleep quality by promoting deeper, non-REM sleep and supporting the nervous system. While it doesn’t address airway issues directly, reducing stress and improving sleep depth can make a big difference in how rested you feel.
Ashwagandha is available in capsules, powders, liquid extracts, and teas. Most people take it earlier in the evening, as it helps with overall stress regulation rather than acting as a sedative.
It’s generally safe for short-term use, but talk to your provider before starting if you take medications or have thyroid issues.
Weight Management
Managing your weight has a direct impact on sleep apnea, especially obstructive sleep apnea. Being overweight, particularly with fat stored around the neck or upper body, increases pressure on the airway and makes it more likely to collapse during sleep.
Losing even a small amount of weight can reduce apnea episodes, improve airflow, and help you get deeper, more restful sleep. Research by Dr. Gary D. Foster from Temple University, Philadelphia, Pennsylvania, USA, found that a 23.8 lbs or 10.8 kg weight loss led to a significant improvement in sleep apnea.
Weight loss also lowers inflammation, improves blood pressure, and supports better overall metabolic health- all important for managing sleep apnea.
The most effective strategies include balanced eating, regular movement, and steady sleep habits. Quick fixes or extreme diets don’t work long-term and can actually disrupt your sleep. If excess weight is a factor, a healthcare provider or a clinical nutritionist can help you build a realistic, sustainable plan.
Frequently Asked Questions
Can Sleep Apnea Cause High Blood Pressure?
Yes, obstructive sleep apnea (OSA) can lead to high blood pressure. The repeated episodes of stopped breathing during sleep cause intermittent hypoxia and interrupted sleep, which activate the sympathetic nervous system, leading to high blood pressure levels. A study by Dr. Tomas Konecny from the Division of Cardiovascular Diseases, Mayo Clinic, Rochester, MN, USA, shows that about 50% of patients with hypertension also have OSA, indicating a strong association between the two conditions.
Is Sleep Apnea Linked To Heart Disease?
Yes, sleep apnea is linked to heart disease. According to Dr. Satya Preetham Gunta from the University of Missouri-Kansas City, Kansas City, Missouri, USA, OSA increases the risk of various cardiovascular conditions, including coronary artery disease, heart failure, and arrhythmias. The intermittent hypoxia and arousals associated with OSA contribute to endothelial dysfunction, inflammation, and increased sympathetic activity, all of which are risk factors for heart disease.
Can Sleep Apnea Lead To Weight Gain Or Make It Harder To Lose Weight?
Yes, sleep apnea can contribute to weight gain and make weight loss more challenging. A study by Dr. Ari Shechter from Columbia University, NY, USA, shows that OSA disrupts normal sleep patterns, leading to hormonal imbalances that increase appetite and reduce energy expenditure. Additionally, daytime fatigue from poor sleep can decrease physical activity levels, further promoting weight gain.
Are Thyroid Disorders Linked To Sleep Apnea?
Yes, hypothyroidism is associated with an increased risk of obstructive sleep apnea (OSA). A study by Dr. Chitranshu Pancholi from the K.G.M.U, Lucknow, Uttar Pradesh, India, found that 74% of hypothyroid patients had OSA, with severity correlating to higher TSH levels. Treating hypothyroidism may reduce OSA symptoms.
Can Sleep Apnea Increase The Risk Of Stroke?
Yes, obstructive sleep apnea (OSA) significantly increases the risk of stroke. The Sleep Heart Health Study by Dr. Susan Redline from Case Western Reserve University, Cleveland, Ohio, USA reported that individuals with severe OSA had a 2.5 times higher risk of ischemic stroke compared to those without OSA. The risk escalates with the severity of OSA.
Conclusion
Sleep apnea is more than just loud snoring. It can affect your heart, weight, energy, and even your mood. Understanding the different types, causes, and symptoms helps you recognize how deeply it can impact your health.
Alongside medical treatments, holistic approaches like chiropractic care, dietary changes, and targeted supplements can support better sleep and breathing. Addressing root causes like inflammation, stress, and weight makes a lasting difference in managing sleep apnea naturally.
You don’t have to settle for restless nights or daytime exhaustion when better options are right here.
At the Bay Clinic of Chiropractic in Panama City, FL Dr. Tony Salamay takes a root-cause approach to sleep apnea. Through personalized care rooted in functional medicine, advanced chiropractic techniques, and clinical nutrition, he helps you improve sleep, reduce symptoms, and feel more in control of your health.
If you’re reading to breathe easier and sleep deeper, reach out. Contact the Bay Clinic of Chiropractic today and find out how we can help you get the rest your body’s been asking for.
References
- Cumpston E, Chen P. Sleep apnea syndrome [Internet]. StatPearls – NCBI Bookshelf. 2023. Available from: https://www.ncbi.nlm.nih.gov/books/NBK564431/
- Bhutta BS, Alghoula F, Berim I. Hypoxia [Internet]. StatPearls – NCBI Bookshelf. 2024. Available from: https://www.ncbi.nlm.nih.gov/books/NBK482316/
- Singareddy R, Bixler EO, Vgontzas AN. Fatigue or daytime sleepiness? [Internet]. 2010. Available from: https://pmc.ncbi.nlm.nih.gov/articles/PMC2919674/
- Slowik JM, Sankari A, Collen JF. Obstructive sleep apnea [Internet]. StatPearls – NCBI Bookshelf. 2025. Available from: https://www.ncbi.nlm.nih.gov/books/NBK459252/
- Rana AM, Sankari A. Central sleep apnea [Internet]. StatPearls – NCBI Bookshelf. 2023. Available from: https://www.ncbi.nlm.nih.gov/books/NBK578199/
- Stuck BA, Hofauer B. The diagnosis and treatment of snoring in adults. Deutsches Ärzteblatt International [Internet]. 2019 Nov 21;116(48):817–24. Available from: https://pmc.ncbi.nlm.nih.gov/articles/PMC6947688/
- Ohayon MM, Guilleminault C, Priest RG, Caulet M. Snoring and breathing pauses during sleep: telephone interview survey of a United Kingdom population sample. BMJ [Internet]. 1997 Mar 22;314(7084):860. Available from: https://pmc.ncbi.nlm.nih.gov/articles/PMC2126255/
- Spałka J, Kędzia K, Kuczyński W, Kudrycka A, Małolepsza A, Białasiewicz P, et al. Morning Headache as an Obstructive Sleep Apnea-Related Symptom among Sleep Clinic Patients—A Cross-Section Analysis. Brain Sciences [Internet]. 2020 Jan 19;10(1):57. Available from: https://pmc.ncbi.nlm.nih.gov/articles/PMC7016602/
- Doyle-McClam M, Shahid MH, Sethi JM, Koo P. Nocturia in women with obstructive sleep apnea. American Journal of Lifestyle Medicine [Internet]. 2018 Jun 18;15(3):260–8. Available from: https://pmc.ncbi.nlm.nih.gov/articles/PMC8120610/
- Schwartz AR, Patil SP, Laffan AM, Polotsky V, Schneider H, Smith PL. Obesity and obstructive sleep apnea: Pathogenic mechanisms and therapeutic approaches. Proceedings of the American Thoracic Society [Internet]. 2008 Feb 4;5(2):185–92. Available from: https://pmc.ncbi.nlm.nih.gov/articles/PMC2645252/
- Mukherjee S, Saxena R, Palmer LJ. The genetics of obstructive sleep apnoea. Respirology [Internet]. 2017 Nov 7;23(1):18–27. Available from: https://pmc.ncbi.nlm.nih.gov/articles/PMC7308164/
- Ceban F, Abayomi N, Saripella A, Ariaratnam J, Katsnelson G, Yan E, et al. Adverse events in patients with obstructive sleep apnea undergoing procedural sedation in ambulatory settings: An updated systematic review and meta-analysis. Sleep Medicine Reviews [Internet]. 2024 Nov 28;80:102029. Available from: https://www.sciencedirect.com/science/article/pii/S1087079224001333?via%3Dihub
- Bland J. Defining function in the functional medicine model [Internet]. 2017. Available from: https://pmc.ncbi.nlm.nih.gov/articles/PMC5312741/
- Birben E, Sahiner UM, Sackesen C, Erzurum S, Kalayci O. Oxidative stress and antioxidant defense. World Allergy Organization Journal [Internet]. 2012 Jan 1;5(1):9–19. Available from: https://pmc.ncbi.nlm.nih.gov/articles/PMC3488923/
- Calder PC. Omega-3 fatty acids and inflammatory processes. Nutrients [Internet]. 2010 Mar 18;2(3):355–74. Available from: https://pmc.ncbi.nlm.nih.gov/articles/PMC3257651/
- Leidy HJ, Armstrong CLH, Tang M, Mattes RD, Campbell WW. The influence of higher protein intake and greater eating frequency on appetite control in overweight and obese men. Obesity [Internet]. 2010 Mar 25;18(9):1725–32. Available from: https://pmc.ncbi.nlm.nih.gov/articles/PMC4034047/
- Asensi MT, Napoletano A, Sofi F, Dinu M. Low-Grade Inflammation and Ultra-Processed Foods Consumption: A review. Nutrients [Internet]. 2023 Mar 22;15(6):1546. Available from: https://pmc.ncbi.nlm.nih.gov/articles/PMC10058108/
- Choe JW, Joo MK, Kim HJ, Lee BJ, Kim JH, Yeon JE, et al. Foods inducing typical gastroesophageal reflux disease symptoms in Korea. Journal of Neurogastroenterology and Motility [Internet]. 2017 Feb 2;23(3):363–9. Available from: https://pmc.ncbi.nlm.nih.gov/articles/PMC5503285/
- Hopper DE, Cramer G. Conservative treatment using chiropractic care and orofacial myofunctional therapy for obstructive sleep apnea: a case report. Journal of Chiropractic Medicine [Internet]. 2023 Jun 22;22(3):234–8. Available from: https://pmc.ncbi.nlm.nih.gov/articles/PMC10461150/
- Office of Dietary Supplements – Vitamin D [Internet]. Available from: https://ods.od.nih.gov/factsheets/VitaminD-HealthProfessional/
- Office of Dietary Supplements – magnesium [Internet]. Available from: https://ods.od.nih.gov/factsheets/Magnesium-HealthProfessional/
- Savage RA, Zafar N, Yohannan S, Miller JMM. Melatonin [Internet]. StatPearls – NCBI Bookshelf. 2024. Available from: https://www.ncbi.nlm.nih.gov/books/NBK534823/
- Tammadon MR, Nobahar M, Hydarinia-Naieni Z, Ebrahimian A, Ghorbani R, Vafaei AA. The effects of valerian on sleep quality, depression, and state anxiety in hemodialysis patients: a randomized, double-blind, crossover clinical trial. Oman Medical Journal [Internet]. 2021 Mar 15;36(2):e255. Available from: https://pmc.ncbi.nlm.nih.gov/articles/PMC8077445/
- Saadatmand S, Zohroudi F, Tangestani H. The effect of oral chamomile on anxiety: A systematic review of clinical trials. Clinical Nutrition Research [Internet]. 2024 Jan 1;13(2):139. Available from: https://pmc.ncbi.nlm.nih.gov/articles/PMC11109927/
- Cheah KL, Norhayati MN, Yaacob LH, Rahman RA. Effect of Ashwagandha (Withania somnifera) extract on sleep: A systematic review and meta-analysis. PLoS ONE [Internet]. 2021 Sep 24;16(9):e0257843. Available from: https://pmc.ncbi.nlm.nih.gov/articles/PMC8462692/
- Foster GD. A Randomized Study on the Effect of Weight L: The Sleep AHEAD Study. Effect of Weight Loss on Obstructive Sleep Apnea. Archives of Internal Medicine [Internet]. 2009 Sep 28;169(17):1619. Available from: https://pmc.ncbi.nlm.nih.gov/articles/PMC2879275/
- Konecny T, Kara T, Somers VK. Obstructive sleep apnea and hypertension. Hypertension [Internet]. 2013 Dec 31;63(2):203–9. Available from: https://pmc.ncbi.nlm.nih.gov/articles/PMC4249687/
- Gunta SP, Jakulla RS, Ubaid A, Mohamed K, Bhat A, López-Candales A, et al. Obstructive Sleep Apnea and Cardiovascular Diseases: Sad Realities and Untold Truths regarding Care of Patients in 2022. Cardiovascular Therapeutics [Internet]. 2022 Aug 11;2022:1–10. Available from: https://pmc.ncbi.nlm.nih.gov/articles/PMC9388301/
- Shechter A. Obstructive sleep apnea and energy balance regulation: A systematic review. Sleep Medicine Reviews [Internet]. 2016 Jul 16;34:59–69. Available from: https://pmc.ncbi.nlm.nih.gov/articles/PMC5237615/
- Pancholi C, Chaudhary SC, Gupta KK, Sawlani KK, Verma SK, Singh A, et al. Obstructive Sleep Apnea in Hypothyroidism. Annals of African Medicine [Internet]. 2022 Oct 1;21(4):403–9. Available from: https://pmc.ncbi.nlm.nih.gov/articles/PMC9850883/
- Redline S, Yenokyan G, Gottlieb DJ, Shahar E, O’Connor GT, Resnick HE, et al. Obstructive Sleep Apnea–Hypopnea and incident stroke. American Journal of Respiratory and Critical Care Medicine [Internet]. 2010 Mar 26;182(2):269–77. Available from: https://pmc.ncbi.nlm.nih.gov/articles/PMC2913239/